 Society
Society

 |
| A doctor examines and gives consultancy on stroke prevention for a patient in Hà Nội. — VNA/VNS Photo Minh Quyết |
HÀ NỘI — A stroke is no longer a disease confined to the elderly. Patients are getting younger and the attacks are striking more unexpectedly, with most still missing the golden hour, the most critical window for effective treatment.
At the Stroke Unit under the Emergency and Intensive Care Ward of Hà Nội Medical University Hospital, every passing minute can determine a patient’s chance of recovery.
Sitting quietly on a bench in the corridor of the Stroke Unit, Nguyễn Thị Từ, 68, from Thường Tín Commune in Hà Nội, could not take her eyes off the door of the patient’s room.
Behind it, her husband was fighting for his life after a sudden stroke that developed within just a few hours.
"That whole night, I barely slept," Từ said, her voice still trembling.
"Around 9pm on April 10, he complained of a headache. I thought it was just fatigue, so I told him to lie down and rest and gave him some medicine. But by midnight, it hadn’t improved. He became drowsy, spoke unclearly and vomited a lot. That’s when the family truly panicked and called an ambulance to take him to the emergency room."
For Từ, those few hours felt like a nightmare.
"I never thought a stroke could come so quickly. Before that, he was living normally. But after just one night, everything changed completely. Now I just hope he gets through the critical phase, can speak again, walk again... that would be a relief," she said.
But not everyone is so fortunate.
Quyền, 70, lives in Khương Thượng Ward in Hà Nội and initially dismissed symptoms such as limb paralysis and slurred speech as signs of ageing.
It was not until a day later, when his condition worsened, that he was hospitalised.
Diagnosis revealed extensive cerebral infarction accompanied by arrhythmia. By then, the “golden hour” had passed. Treatment had to be prolonged, involving multiple specialities, and the prognosis for recovery became far more difficult.
Doctors said cases like Quyền’s, arriving late at hospital, are not uncommon. This is partly due to poor public recognition of stroke symptoms and partly due to complacency, hesitation or reliance on unverified folk remedies.
Life measured in minutes
In the battle against stroke, time is the decisive factor. On the front line of emergency care, doctors work in a continuous race where every minute can alter a patient’s fate.
Doctor Vũ Đình Hùng from the Stroke Unit told Sức khỏe & Đời sống (Health and Life) newspaper that at Hà Nội Medical University Hospital, the emergency system operates continuously, with no distinction between day and night, always ready to receive acute stroke patients.
According to statistics, the unit treats more than 1,000 stroke cases each year. Cases are not concentrated at fixed times but occur throughout the 24-hour cycle.
"Our working day does not start with office hours but with the Code Stroke signal, the red alert for an urgent stroke emergency. When this signal is activated, the entire team, from emergency doctors, neurologists, to nurses, immediately coordinates, racing against time to seize back the patient’s chance of survival," Hùng said.
The period from midnight to early morning is often the most critical. Many patients notice symptoms upon waking, making it difficult to determine the onset time, which in turn affects treatment decisions.
Hùng said that in stroke care, not only medical staff but also patients’ relatives play a pivotal role as the decision to act quickly or delay in the first minutes can determine the difference between recovery and lifelong disability.
25 decisive minutes
Hùng said that once a stroke is identified, emergency protocols are activated immediately in a race against time.
“Upon arrival, the patient was suspected of having a stroke, and we initiated Code Stroke. We performed clinical examination, blood tests and urgent imaging. The entire process, from admission to imaging results, typically takes about 25 minutes,” he said.
Following the initial assessment, doctors from emergency, neurology, interventional and cardiology teams consult rapidly to determine the most appropriate treatment plan. Depending on the case, patients may receive thrombolytic therapy, undergo thrombectomy, or require surgery.
Hùng said three key factors determine survival and recovery from stroke.
First is the pre-hospital response: relatives must recognise the signs early and rush the patient to a medical facility, avoiding unverified folk remedies.
Second is the onset time. “Time is brain.” Within the first 4.5 hours, thrombolytic therapy may be administered, and in some cases of large-vessel occlusion, intervention may be possible up to 24 hours.
Third is multidisciplinary coordination, as stroke is not confined to a single speciality, he said.
The Hà Nội Medical University Hospital has also deployed artificial intelligence in stroke emergency care.
"We have applied AI in patient triage from the reception stage, helping to quickly identify suspected stroke cases for priority treatment. In imaging diagnosis, modern machines and software can analyse lesion areas and ischaemic regions, assisting doctors in making more accurate decisions," Hùng said.
He said applying technology not only shortens the time from hospital arrival to intervention but also improves treatment accuracy.
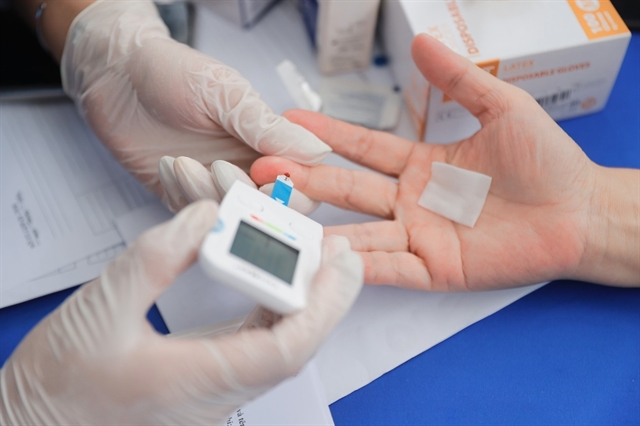 |
| A medical worker takes blood glucose sample for testing. Maintaining stable blood glucose significantly reduces the risk and improves the prognosis of stroke. — VNA/VNS Photo Minh Quyết |
Despite intensified public awareness campaigns on stroke recognition and management in recent years, reality at medical facilities shows many patients still miss the golden hour, the critical window that determines treatment effectiveness.
Doctor Hùng noted that the biggest barrier is not technique or equipment, but patients arriving too late. Many early symptoms, such as facial droop, limb weakness or slurred speech, go unrecognised, or families hesitate, monitor the condition or attempt self-treatment at home.
"Currently, the rate of patients arriving within the intervention window is under 30 per cent. Many cases involve family hesitation or incorrect initial handling, forfeiting the best treatment opportunity," he said.
Therefore, Hùng believes raising community awareness must go beyond recognising symptoms to understanding urgency and acting immediately by calling emergency services or taking the patient to the nearest stroke-capable facility.
Younger patients
Another worrying reality is the clear trend of stroke affecting younger people, no longer an “elderly disease” as before.
Doctor Hùng said modern lifestyle changes are a primary cause. Work pressure, prolonged stress and unhealthy habits such as staying up late, lack of exercise, alcohol and smoking are silently increasing risk factors among younger people.
"In my view, there are two main causes. First is the modern lifestyle with pressures, unhealthy routines, rising obesity and chronic diseases in the young. Second is advanced diagnostics detecting more strokes in young people than before," he said.
Clinical records show many very young stroke patients, even in their 20s. This not only impacts individual health but also brings economic and social consequences, as patients are often of working or studying age.
Doctor Hùng advises that, alongside early screening for risk factors, young people should adopt healthy lifestyles, maintain physical activity, control weight, limit stimulants and undergo regular health checks.
Most importantly, at any suspected sign of stroke, patients should seek hospital care immediately to avoid missing the golden hour. — VNS




