 Society
Society

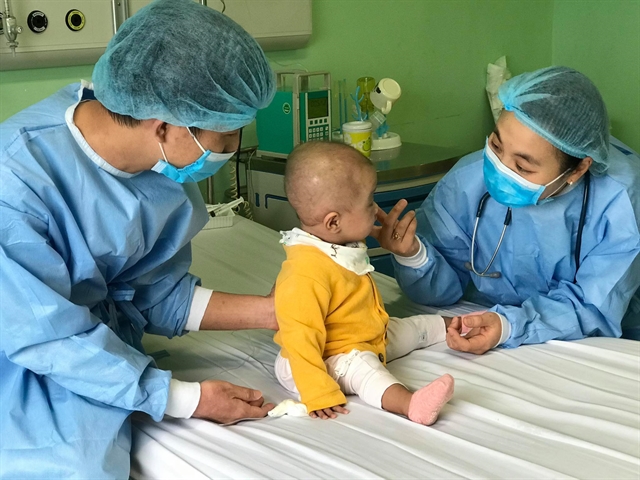
Doctors from two major hospitals in Việt Nam help treating a child patient who suffered from innate combined immunodeficiency.
|
| The child patient spent a whole year in hospitals to fight her serious illness of innate combined immunodeficiency and other diseases. — Photo from the Ministry of Health |
HÀ NỘI — It’s always a bold decision to conduct a bone marrow transplant to save a baby who suffers from combined innate immunodeficiency and many other diseases.
The success rate of the stem cell transplant is just 10-20 per cent, but without the transplant, the baby would die before they turn a year old, said Associate Professor and Dr Trần Minh Điển, deputy director of the National Children's Hospital.
According to health experts, immunodeficiency is a genetic defect that makes the child's body unable to fight off pathogens such as viruses and bacteria. Therefore, children often get serious, persistent or recurrent infections. Depending on the type of immunodeficiency type, patients will develop different infections.
Thiên Ngọc, a baby girl born in late 2019 in the southern province of Đồng Nai was diagnosed with combined innate immunodeficiency when she was around three months old.
Doctors at HCM City-based Children's Hospital No.2 came to that inclusion after treating her for repeated diarrhoea, sore throat and pneumonia.
At times, when the child recovered and was set to be discharged, she suffered a fever again, said Trần Quỳnh Hương, head of the Respiratory Department at the hospital – who examined and treated the baby.
In February 2020, Hương for the first time contacted doctor Nguyễn Ngọc Quỳnh Lê from the Department of Immunology-Allergy-Arthritis at Hà Nội-based National Children's Hospital to discuss the case.
For the following three months, they called each other regularly to talk about the child’s conditions, discussing possible treatment and tests as well as seeking a healthcare unit that could offer a stem cell transplant for the baby.
At that time, a bone marrow transplant was identified as the only way to save the baby. With the advanced technique, stem cells from a healthy donor that are genetically suitable to the recipient would be taken and replace the dysfunctional stem cells.
Bone marrow transplant (hematopoietic stem cell transplant, or HPSCT) involves the administration of healthy hematopoietic stem cells in patients with dysfunctional or depleted bone marrow. This helps to augment bone marrow function and allows, depending on the disease being treated, to either destroy tumour cells with malignancy or to generate functional cells that can replace the dysfunctional ones in cases like immune deficiency syndromes, hemoglobinopathies, and other diseases.
“It was a challenge for both doctors and the patient’s family as in Việt Nam, only the National Children's Hospital has sufficient equipment and experience to conduct the transplant,” Hương said.
Transferring a patient from HCM City to Hà Nội during the pandemic was not easy, while the medical cost would be far out of reach for the patient’s family.
“Seeing Lê’s enthusiasm and the chance to save the baby, we had the motivation to work with relevant parties to speed up the patient transfer and transplant,” doctor Hương said.
In late May 2020, the baby’s health condition worsened and doctors from the two hospitals – one in the south and the other in the north – had an online meeting.
Deputy director of National Children's Hospital Điển said they were bold to receive the child with such serious health conditions.
“The success rate is only ten to 20 per cent while few such successful transplants were recorded in the world,” he said.
Doctor Hương from HCM City’s Children's Hospital said that doctors not only completed insurance procedures for the baby but also called on donations for transferring her to Hà Nội and covering costs that health insurance did not cover. The patient’s family at that time could afford only VNĐ700 million (over US$30,000) while the medical cost for such a transplant could reach billions of Vietnamese đồng.
On May 29, 2020, Hương and a nurse escorted the child to Hà Nội on a Vietjet flight thanks to the airline operator ensuring proper medical and security conditions amid the ongoing COVID-19 pandemic in the country.
Hương said that when arriving at the National Children's Hospital, the child was suffering from severe pneumonia that required supplemental oxygen, tuberculosis complications, diarrhoea caused by Rotavirus, rectal prolapse due to prolonged diarrhoea, and severe malnutrition.
It took two months to improve the baby’s health so that she would be healthy enough to undergo the first stem cell transplant.
Nguyễn Thanh Bình, vice head of the Blood Testing Department at the National Children's Hospital said that the hospital took bone marrow from the baby’s mother for her transplant after finding no suitable bone marrow donor.
“Previously, the hospital succeeded in conducting such transplants,” Bình said, adding that the technique was complicated and costly in which only stem cells and good cells were kept while bad cells which cause harmful reactions would be removed.
As the baby was in poor health, using chemicals to kill marrow could put the baby at risk of many complications, even death, doctor Chi said.
After discussing with experts from Hong Kong and reviewing foreign medical records, doctors decided to conduct two bone marrow transplants for the baby.
The first transplant using no chemicals aimed to revive part of the baby’s immune system to help her fight against bacterial infections. The second transplant would use chemicals under treatment protocol to kill all the baby's faulty hematopoietic stem cells and transfer the mother's healthy stem cells to the baby.
The first transplant was conducted on July 22, 2020. After that, the baby got a high fever and diarrhoea for four straight weeks, Chi said, adding that they were thinking the transplant had failed.
However, continuing efforts were made to save the baby. She gradually recovered from the fifth week, with no fever and diarrhoea.
The second transplant was conducted on November 23, 2020 – three months after the first one.
Undergoing intensive care for a month after the second stem cell transplant, the child patient did not have any complications. Results showed that the mother’s stem cells are growing well inside the baby.
“All hardships, difficulties and stress we faced when treating her seemingly disappeared, the baby is healthy, has gained weight and is very active,” doctor Lê said.
Spring seemed to come early to the doctors and the baby’s family since the moment she was announced as not having the life-threatening illness – combined immunodeficiency – anymore. — VNS




