 Society
Society

Closer collaboration among stakeholders is needed to improve access to innovative medicines to combat cancer in ASEAN member countries, experts have said.
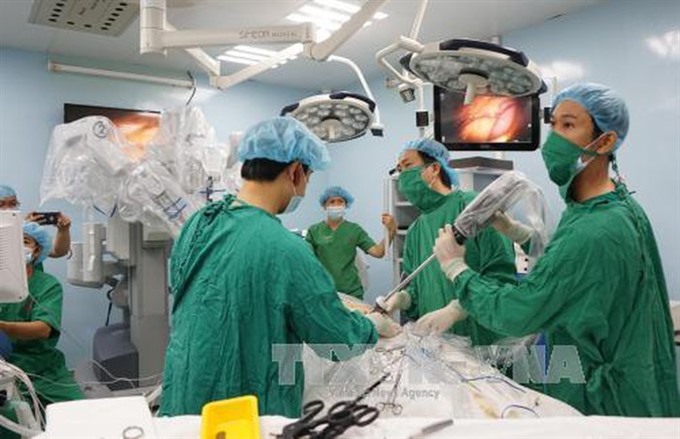 |
| Doctors perform surgery on a patient with stomach cancer.— VNA/VNS Photo Phương Vy |
By Thu Ngân
HCM CITY — Closer collaboration among stakeholders is needed to improve access to innovative medicines to combat cancer in ASEAN member countries, experts have said.
At the current dialogue session “Taking Action Together: Improving Care for Cancer Patients in ASEAN countries” at the 2018 World Cancer Congress held in Malaysia by the Union of International Cancer Control and Bayer, experts said the public and private healthcare sectors and NGOs had to collaborate closely to combat access barriers to innovative cancer medicines in Southeast Asia.
The session heard that many people in the region lacked adequate access to cancer care, and the challenges faced by countries over access to medicines were multi-faceted and required contributions from all stakeholders.
There was a clear need for governments to extend financial protection through social health insurance and publicly-supported cancer care to relieve patients from the cost burden of cancer treatment.
Patient-assistance programmes (PAP) supported by companies together with partners from local healthcare systems and NGOs would also help close such healthcare gaps.
For instance in Viet Nam, Bayer sponsored a PAP managed by the Bright Future Fund (BFF), a member of the Union of International Cancer Control, to provide patients suffering from hepatocellular carcinoma or advanced renal cell carcinoma with better access to first-line oral targeted therapy.
Approved by the Ministry of Health, the PAP was launched in 2016, and it has since provided partial funding to patients who are diagnosed with HCC or RCC, and are prescribed with the targeted oral cancer drug.
In its first year, the PAP supported 852 HCC patients and 52 RCC patients in 19 hospitals and medical centres.
At the dialogue session, experts also said though more people were diagnosed with cancer, the good news was that innovative cancer medicines along with better care were helping cancer patients live longer and better.
Over the past few decades the death rates of many cancers had fallen, reducing it from a death sentence to a chronic condition, and many were even cured.
Better treatment and improved survival mean people were able to return to their usual daily routines, resume work and play an active role in society and the economy.
In the 1970s fewer than half the people with cancer survived five years. Today two out of three people survive at least five years.
New therapies had contributed to significant declines in cancer death rates around the world since its peak in 1991. Approximately 73 percent of survival gains in cancer were attributable to new medicines.
Cancer treatment had evolved from pain palliation to chronic management, with targeted therapies which halted or slowed down disease progression, minimised complications, improved the quality of life, prevented hospitalisation and surgeries, reduced side effects, and even cured.
New, innovative cancer treatment offered hope to patients who had limited or no other options. Incremental advances in cancer treatment made a huge difference to patients who did not respond to currently available treatments.
Adding multiple lines of treatments could help cancer patients extend their lives and improve the quality of their lives.
For example, in hepatocellular carcinoma, where survival rates were low, the approval of the first oral targeted therapy for first-line systemic treatment of HCC in 2007 represented new hope for many patients.
As many patients still experienced disease progression, there remained an unmet need for the development of additional treatments for HCC.
This supported the recent approval of a second-line oral targeted therapy around the world.
Both first- and second-line therapies formed a proven systemic treatment sequence to significantly improve overall survival of patients with HCC.
An unprecedented median survival time of 26 months from the start of prior the first-line treatment had been achieved in clinical studies, demonstrating how sequential treatment of two innovative cancer medicines could lead to incremental improvements in survival.
The session also heard that cancer policies and awareness in ASEAN nations differed from country to country since local healthcare systems were unique.
In particular, there was little uniformity when it came to frameworks for access to innovative cancer medicines, leading to delays and access disparities for patients across ASEAN countries.
There were also gaps in knowledge and awareness of cancer among the general public, lack of alignment in care priorities and delivery infrastructure and a lack of early diagnosis and in enhancing treatment outcomes.
In some countries, there was still room for improvement in reimbursement frameworks and decision processes to support the effective use of medicines to treat clinically-eligible patients, ultimately avoiding treatment delays and substantial loss of life years.
Furthermore, there were disparities in health plans that did not cover – or only partially covered –the provision of cancer drugs, while some price control mechanisms and policies could also result in restricted patient access.
Consequently, some patients found themselves having to pay for all expenses out of their pocket, despite the majority not having sufficient funds to cover their treatment.
In Việt Nam, non-communicable diseases accounted for 72 per cent of mortality in 2010, including 29 per cent due to cancer.
Việt Nam has undertaken initiatives to tackle the growing cancer incidence, addressing problems such as a lack of early screening and putting an emphasis on public knowledge of the disease.
In order to support Vietnamese cancer patients, especially patients with liver cancer, the Liver Cancer Patient Support Programme, managed and implemented by the BFF and sponsored by Bayer, was launched. In the programme, patients diagnosed with HCC or RCC and prescribed the targeted oral cancer drug approved by the MOH have half the cost of the oral cancer treatment subsidised. This programme has been implemented nation-wide since early 2017 with 19 hospitals taking part. To sign up for the programme, HCC patients can contact doctors at hospitals taking part in it. Consultants at these hospitals will provide details. Patients can also contact Ms. Nguyen Ha My at 84 91 393 6658 or call the BFF office at +84 24 6680 6969 or email quyngaymaituoisang@gmail.com for further support. This is one of the long-term programmes to help HCC patients with the treatment cost and enables them to follow the treatment process so that they can optimise treatment response and prolong their lives. |




