 Society
Society

|
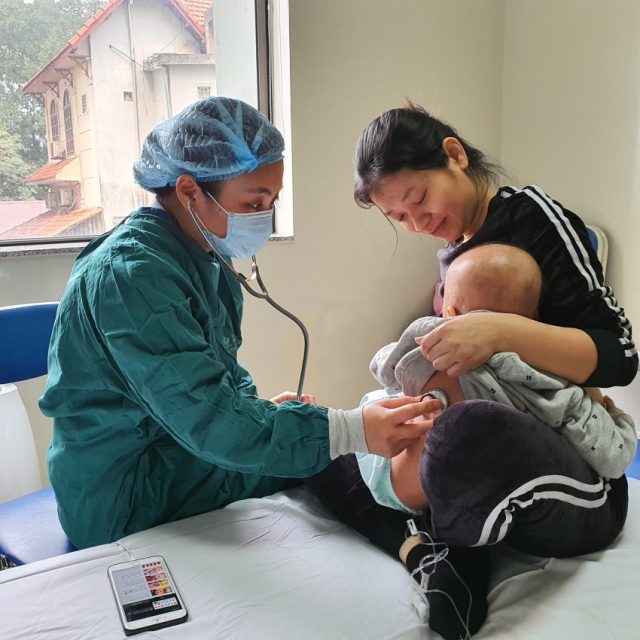
| Doctor Nguyễn Ngọc Quỳnh Lê checks the health of WAS child patient after the stem cell transplant. — Photo benhviennhitrunguong.org.vn |
HÀ NỘI – The Central Paediatrics Hospital on Tuesday announced that for the first time, its doctors successfully used a bone marrow transplant to cure a two-year-old boy who suffers from Wiskott-Aldrick syndrome (WAS) – a rare disease that affects up to nine people in a million.
WAS is a rare disease characterised by eczema, thrombocytopenia (low platelet count), immune deficiency, and bloody diarrhoea.
Children with the potentially life-threatening, inherited immune system deficiency have difficulty producing platelets, the blood component that fosters clotting, which leaves them susceptible to bleeding. Their compromised immune systems leave them susceptible to infections, eczema, autoimmunity and cancer.
According to the Central Paediatrics Hospital, the bone marrow or stem cell transplant for the toddler took place on February 26 with stem cells donated from his older sister.
One week before the transplant, the toddler underwent chemotherapy to destroy his diseased bone marrow and make room for new, healthy cells.
The child’s parents said that when he was one-day old, bleeding spots appeared on his belly and doctors from Quảng Ninh Hospital for Mother and Children examined and transferred him to the Central Paediatrics Hospital in Hà Nội.
He was in the hospital for a week and then returned home to the northeastern province of Quảng Ninh as results showed indicators were normal.
However, on a visit to the hospital in September last year, doctors found that his platelets were low plus he had bloody diarrhoea and bleeding spots on skin.
“My family was shocked to hear that my son had a rare disease. It’s so rare that we cannot remember and pronounce its name exactly,” the patient's father said, adding that they had lost a child to the same symptoms six years ago, but at that time they were not aware of the disease.
Milestone
Dr Nguyễn Ngọc Quỳnh Lê from the hospital’s Immune - Allergy - Joints Department said that doctors closely monitored and treated the boy since he was diagnosed.
After consulting his parents about stem cell transplant and screening his relatives to find suitable stem cells, doctors found that an ideal cell donor was his older sister.
“Thanks to careful preparation and smooth co-operation of the surgical team, the patient did not have any series complication after the transplant. Post-surgery complications like fever, mucositis or graft-versus-host disease – which occurs when the donor’s grafted cells react against the host patient’s cells – were detected quickly and controlled properly,” Lê said.
Twenty-one days after the transplant, the new cells developed in the child patient at a rate of 87 per cent, while his blood index turned normal.
Thirsty-three days after the transplant, the rate reached 100 per cent, proving the success of the transplant.
Lê said that people with WAS usually can live for a maximum of five years and the only treatment available now was stem cell transplant when new, healthy cells were put into the patients’ bloodstream.
Lê Quỳnh Chi, head of the Immune-Allergy-Joints Department said that stem cell transplant for a WAS patient marked a milestone in the hospital’s treatment. Until now, the stem cell transplant has been used for patients with marrow failure, Thalasemia and innate immunodeficiency.
Now, there are 11 child patients with WAS in the hospital.
“Stem cell transplants can help save them, but the cost for a transplantation is high, ranging from hundreds of millions of Vietnamese đồng to VNĐ 1-2 billion, she said.
Heath insurance covered part of the medical costs, so the patients’ families really need financial support, she said. — VNS




