 Society
Society

Việt
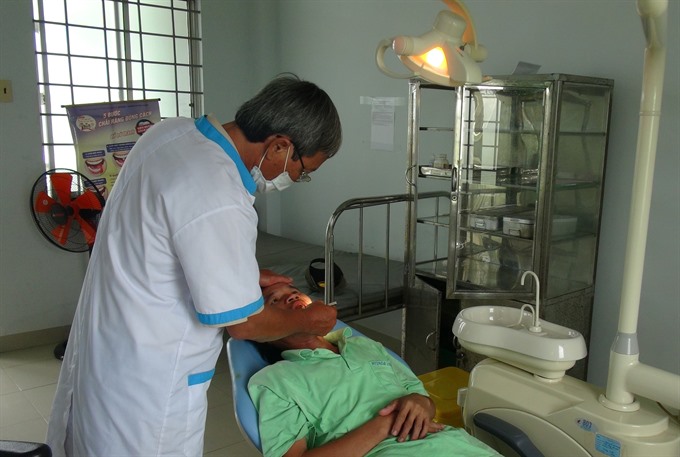 |
| A man receives a health check at Ninh Quang Commune’s Health Station in Ninh Hòa Town in central Khánh Hòa Province. — VNA/VNS Photo Phan Sáu |
HÀ NỘI — Việt
The Health Ministry and the World Health Organisation (WHO) discussed the problem in Hà Nội on Tuesday at their first meeting to discuss improving primary healthcare to gain universal health coverage (UHC). UHC means ensuring that all people can access essential quality health services without facing financial hardship.
Phan Lê Thu Hằng, deputy general director of the planning and finance department under the health ministry, said that grassroots healthcare had always been the foundation for implementing primary healthcare nationwide.
Việt
By 2012, the country had 622 district hospitals with nearly 69,000 beds, 651 regional general clinics with 6,752 beds and over 11,100 commune health stations (CHS).
As many as 73.5 per cent of CHS have doctors, 96.4 per cent of CHS have midwives or assistant doctors in obstetrics and pediatrics and 73.4 per cent of CHS meet national standards on communal level healthcare.
Among over 11,000 CHS nationwide, nearly 3,200 are in need of total rebuilding and nearly 3,600 need upgrading.
“Investment in the development of the grassroots healthcare network so far has not matched the need,” Hằng said.
Other challenges facing Việt
CHS are providing 60 per cent of their assigned technical services, mostly due to a lack of staff or untrained staff and a lack of equipment.
In addition, people lacked awareness on disease prevention and using health services appropriately.
People, especially those living in urban areas with many available heath care institutions, prefer hospitals to ward healthcare stations. The CHS are usually preferred in rural or remote disadvantaged areas and by poor people who cannot access or afford healthcare services at major hospitals.
Health Deputy Minister Phạm Lê Tuấn said that inequities in primary healthcare remained large among urban and rural areas and between the Kinh group and other ethnic groups.
Tuấn said that funding for further developing the grassroots healthcare network faced a bottle-neck while the medical costs at CHS paid by national Health Insurance remained very low.
Less than 4 per cent of the country’s health insurance fund is allocated to the grassroots healthcare network. From 2004-2014, less than 20 per cent of patients in Việt
In Việt
When people must pay directly to the healthcare provider without support from a third-party or Government insurer, they face a great risk of falling into poverty.
Solutions
Deputy General Director of Planning and Finance Department Phan Lê Thu Hằng said that Việt Nam had policies and programmes to strengthen the grassroots healthcare network, but more should be done.
For example, the country should develop a payment system to better link payment to service quality; enhance investment in infrastructure, equipment and medicines and promote staff capacity building, training, technology transfer and staff rotation.
For universal health insurance, the premium should be adjusted appropriate to the economic condition of users and the quality of services. Health insurance packages should be diversified. Linkages and cooperation between social health insurance and commercial health insurance should be strengthened. Synchronous measures are needed to control insurance abuse and fraud and to ensure the health insurance fund is balanced.
Momoe Takeuchi, team leader of WHO’s Health System Development group, said that the health insurance allocation to primary health care providers should be increased to 30 per cent of total health insurance funds over the current 4 per cent.
“This level of funding is a crucial step in obtaining universal health coverage in other countries like
She called for revision of the current list of services and medicines to better reflect the activities and roles of primary healthcare providers. The payment rate to providers should be based on their activities and performance.
The WHO expert also recommended Việt

.jpg)







